Bravehearts of the Foundation: Vijitha
September 25, 2018 | Contributed by R Srivatsan
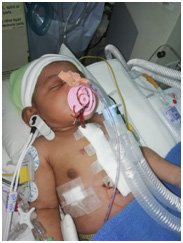
This 2-day old baby girl was born to parents Renjith Kumar and Vijitha in the district of Pattanamthitta on 29th August 2018. Second born to the couple, baby of Vijitha was diagnosed with congenital heart disease antenatally at the ninth month of the pregnancy, even before she was born.
During the mother’s pregnancy, the doctor at the local diagnostic center detected increase heart rate in fetus in a routine checkup. Concerned about a possible heart defect in the fetus, the doctor advised the parents to get a Fetal Echocardiogram—a test similar to an ultrasound, providing better visibility on the unborn baby’s heart function.
Dr. Saji Philip, the Fetal Echo expert at Parumala Hospital, first diagnosed the baby with a heart defect. Immediately consulting with Dr. Balu Vaidyanathan in Amrita Institute of Medical Sciences (AIMS), Dr. Saji Philip referred the parents to AIMS for further care and management.
The baby’s parents and 4-year-old elder brother were worried about her health. On top of that, father Renjith, a casual worker with a meager earning of Rs. 38,000 a year, was struggling to imagine how he would support the costly medical expenses ahead of them.
At AIMS, Dr. Balu confirmed Dr. Saji’s diagnosis and the baby’s delivery was planned under the Obstetrics and Gynecology Department. When the baby was born stable and at a weight of 3.6 kgs, the family was momentarily relieved. However, soon after the delivery the baby became cyanotic. Emergency tests confirmed that the baby had a double outlet right ventricle, large subpulmonic VSD (Taussig Bing anomaly) with hypoplastic aortic arch, severe coarctation of the aorta, and duct dependent lower body perfusion. She was stabilized with prostaglandin infusion and a surgery was planned for the 6th day of her life.
Her surgery was done under cardiopulmonary bypass (CPB). It was initiated by cannulating the innominate artery through a chimney graft. During the surgery the pulmonary artery was routed to the left ventricle by a pericardial patch, closing the ventricular septal defect (VSD). She was then cooled to 18 degrees and circulation was maintained only through the innominate artery (selective cerebral perfusion).
After this her aortic arch was opened, Patent Ductus Arteriosus (PDA) was divided and ductal tissue was removed. Her aortic arch was then repaired by an extended end to end anastomosis by connecting the descending aorta to the undersurface of the aortic arch. Following this, her circulation could finally be maintained in the lower body. Then an arterial switch was done to connect her aorta back to her left ventricle and the pulmonary artery to the right ventricle. She came off bypass smoothly with minimal supports and her chest was closed in layers.

